Chronic pancreatitis, a long-standing inflammation of the pancreas, is often managed first with medication, dietary adjustments, and careful monitoring.
However, in some individuals, the pancreas may gradually undergo structural changes as repeated inflammation affects the gland over time. These changes can impair digestion or lead to persistent complications that no longer respond well to conservative treatment.
When this happens, chronic pancreatitis surgery may be considered to address the underlying problems within the pancreas.
In Singapore, Digestive & Liver Surgery offers several surgical approaches for managing chronic pancreatitis, depending on the underlying cause and the extent of pancreatic damage.
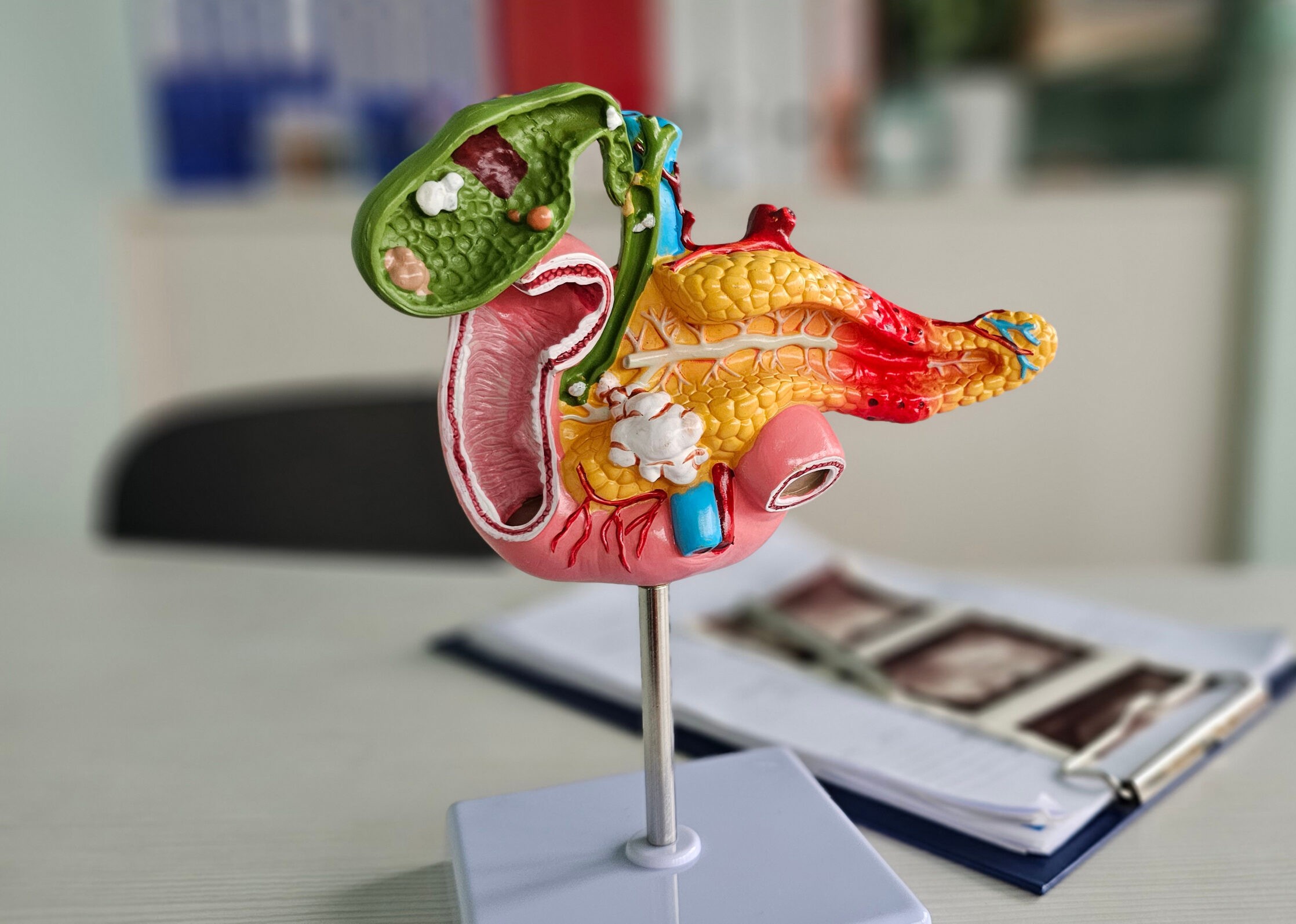
Surgical intervention for chronic pancreatitis is typically recommended when structural damage to the pancreas results in ongoing symptoms or complications that are not adequately controlled with medical management.
Chronic pancreatitis surgery may be indicated in cases involving:

Here are the surgical methods we offer at Digestive & Liver Surgery for the treatment of chronic pancreatitis.
If you have chronic pancreatitis and experience persistent abdominal pain, it may be due to an inflammation that affects nearby nerve pathways.
Nerve-block surgery focuses on reducing these pain signals by targeting the celiac plexus, a group of nerves located close to the pancreas.
During the procedure, the surgeon carefully locates this nerve bundle and interrupts the pain pathways. This is typically done by dividing or disabling the small nerves that carry pain signals from the pancreas to the brain.
As the pancreas itself is not removed or structurally altered, this procedure is generally less extensive than other forms of pancreatic surgery.
After surgery, you’ll have to stay for recovery, so we can monitor and manage any immediate discomfort.
As your body heals and the nerve pathways are disrupted, you may notice that your abdominal pain becomes less intense. This will allow you to rely less on strong pain medications and gradually return to normal daily activities.
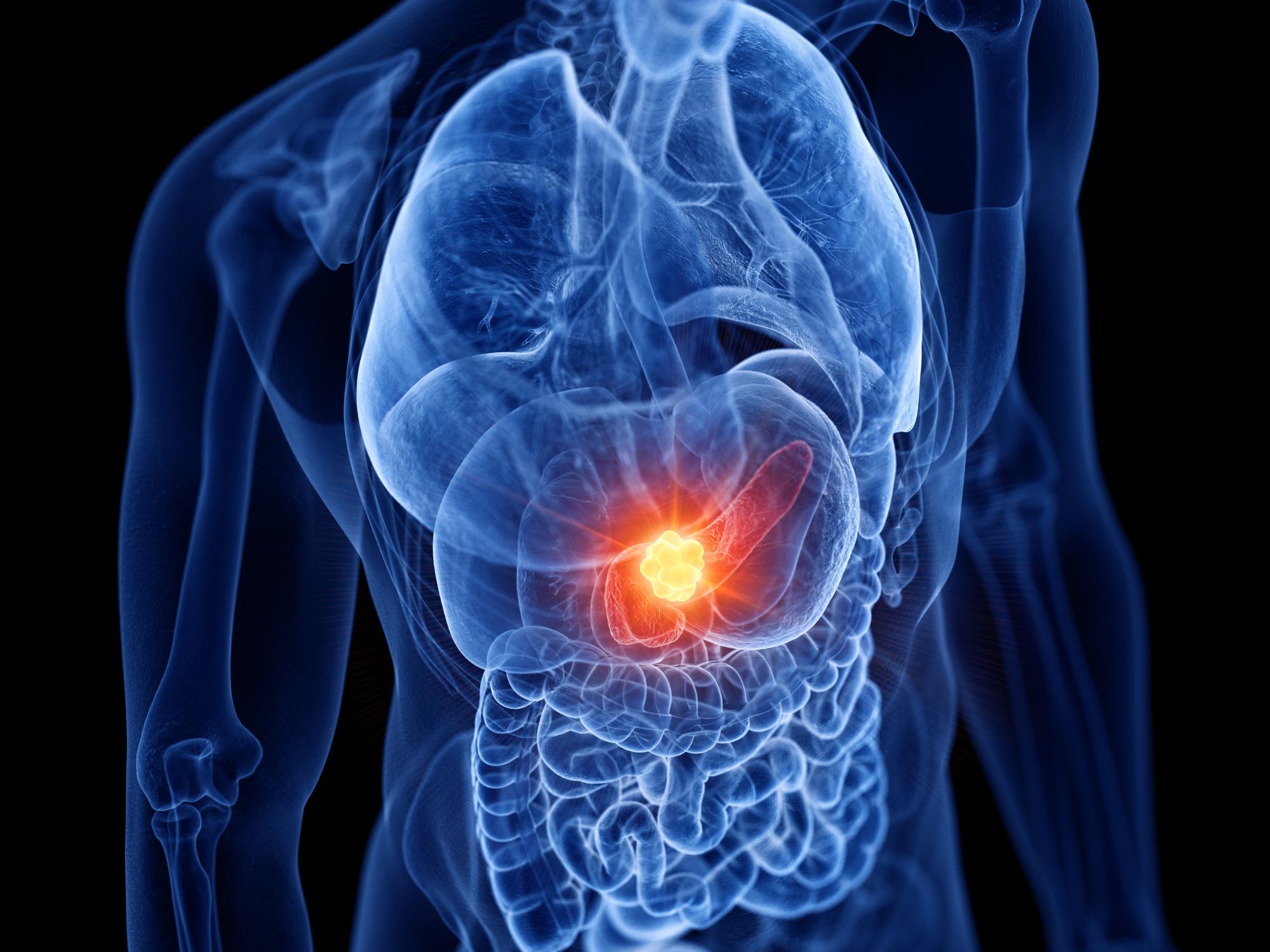
A pancreaticojejunostomy is a drainage procedure used when the main pancreatic duct becomes enlarged or blocked.
When this happens, pancreatic enzymes may not drain properly into the intestine. This can cause pressure to build up within the pancreas and contribute to pain or inflammation.
This procedure improves the drainage of pancreatic enzymes by connecting the pancreatic duct directly to the small intestine.
During the operation:
By improving this drainage, the surgery helps reduce pressure within the pancreas.
After this procedure, you’ll typically be on fluids, allowing your digestive system to adjust, before you’re allowed to eat solid foods again.
You can also gradually return to your daily routine as we monitor your healing and pancreatic function during your follow-up visits.
What type of chronic pancreatitis surgery do you need?
When chronic pancreatitis affects only one part of the pancreas, removing that section of the gland may help relieve symptoms and prevent further complications.
This operation is known as a partial pancreatectomy.
During the procedure:
Because part of the pancreas remains, the body may still be able to produce digestive enzymes and hormones.
After surgery, you may start with fluids before gradually returning to solid foods as your digestive system adjusts. You may also need pancreatic enzyme supplements to help with digestion.
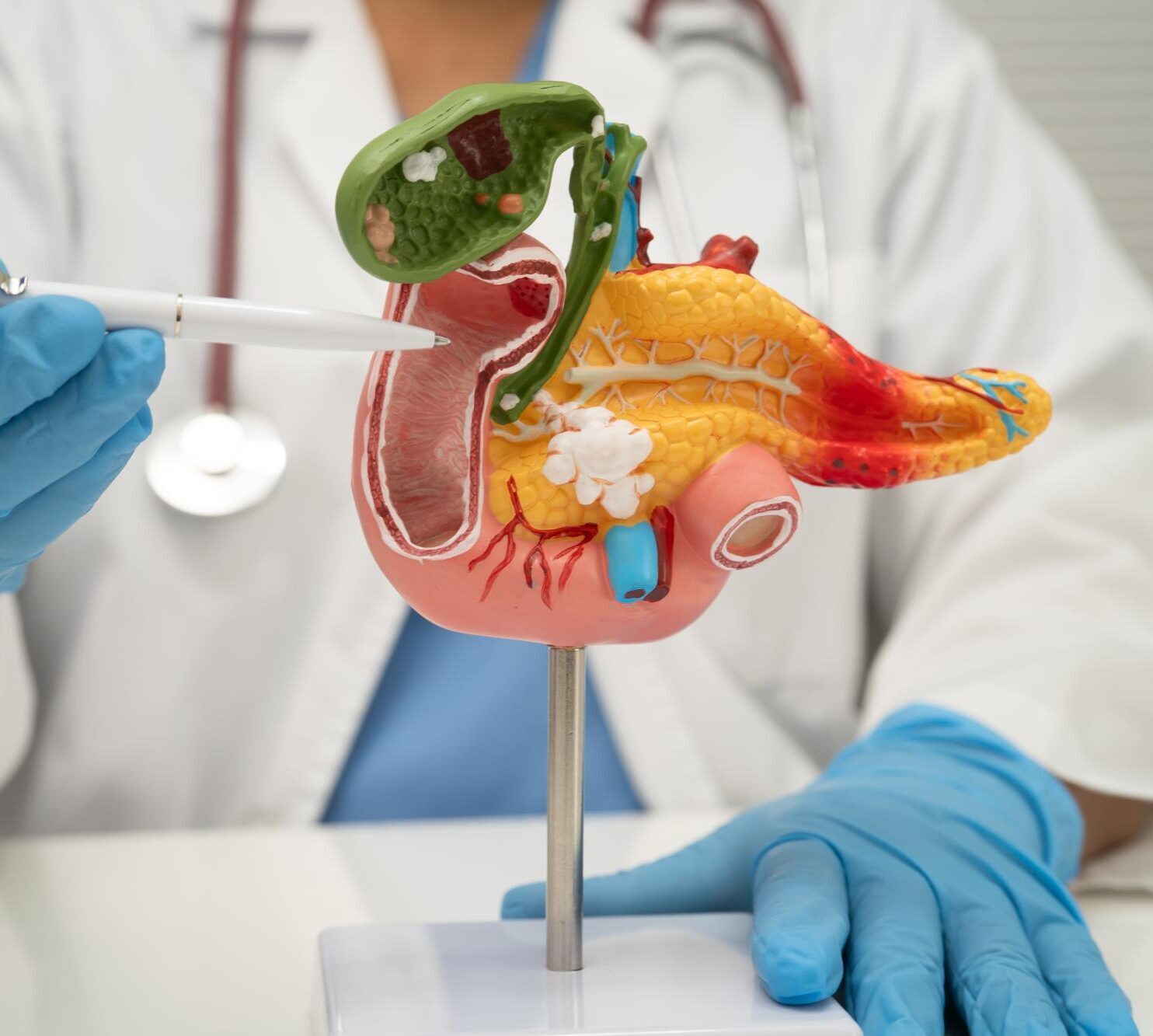
In more advanced cases of chronic pancreatitis, inflammation and scarring may involve the entire pancreas. When other surgical options are unlikely to provide relief, total pancreatectomy may be considered.
This surgery removes the pancreas completely. During the procedure, nearby structures, such as parts of the small intestine or spleen, may also be treated if necessary.
Because the pancreas produces both digestive enzymes and insulin, its removal changes how the body manages digestion and blood sugar.
After surgery, you may need regular treatment to replace these functions, including:

If you suspect you have chronic pancreatitis, speak with a specialist about your treatment options.
During a consultation at Digestive & Liver Surgery, we’ll assess the extent of pancreatic damage and discuss the surgical options that may help manage your symptoms and complications.
Yes, with the right treatment and lifestyle adjustments. Managing chronic pancreatitis often involves medication, dietary changes, and regular medical follow-ups.
Chronic pancreatitis cannot always be stopped completely, but treatment may help slow its progression. Avoiding alcohol, improving your diet, taking necessary medication, and managing various triggers can help protect your remaining pancreatic function.
Surgery usually cannot cure chronic pancreatitis. It’s typically used to treat complications caused by the condition. Depending on your situation, chronic pancreatitis surgery can help relieve pain, improve drainage from the pancreas, or remove severely damaged tissue.
No, chronic pancreatitis is generally considered a long-term condition rather than a terminal illness. While the pancreas may develop permanent damage over time, the condition can often be managed with medical treatment, lifestyle adjustments, and in some cases, surgery.
Surgery for chronic pancreatitis may take several hours, with the exact time depending on the type of procedure being performed.
Professional Care You Can trust

New DLS Group Office
We have opened a new administrative office to support our operations.
The address is:
545 Orchard Road
#10-09 Far East Shopping Centre
Singapore 238882
All medical services continue as usual at our four clinics.
Thank you!

Senior Consultant Surgeon

Senior Consultant Surgeon